

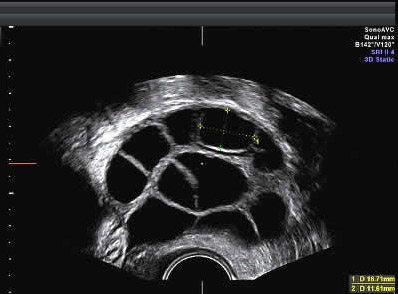
In order to get sufficient eggs for the in vitro fertilization process, the woman is stimulated with injected medications using one of several IVF medication stimulation protocols to develop multiple follicles and egg development. The injections are usually done by the woman, or by her male partner.
The eggs develop in fluid filled structures in the ovaries called follicles. Each follicle can be seen and measured by ultrasound and contains one microscopic egg.
When the woman’s follicles are mature (determined by ultrasound and hormone measurements), the egg aspiration procedure is performed to remove the eggs from the ovaries. Powerful anesthesia medications are given through an IV so that the woman is “out” during the egg retrieval procedure. She will not feel or remember anything. A needle is passed through the top of the vagina under ultrasound guidance to get to the ovary and follicles. The fluid in the follicles is aspirated through the needle and the eggs detach from the follicle wall and are sucked out of the ovary. The actual IVF egg aspiration procedure usually takes 5-10 minutes at our IVF clinic.
The fluid with the eggs is passed to the IVF lab where the eggs are identified, rinsed in culture media, and placed in small culture drops in plastic dishes. The dishes with the eggs are then kept in specialized IVF incubators under carefully controlled environmental conditions.
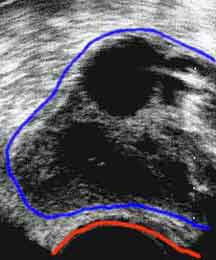
The embryos are cultured in the IVF lab for 2-5 more days in the lab before they are put into the woman’s uterus with the embryo transfer procedure.
Fourteen days after the embryo transfer procedure, we take the woman’s blood to test for HCG, the pregnancy hormone.
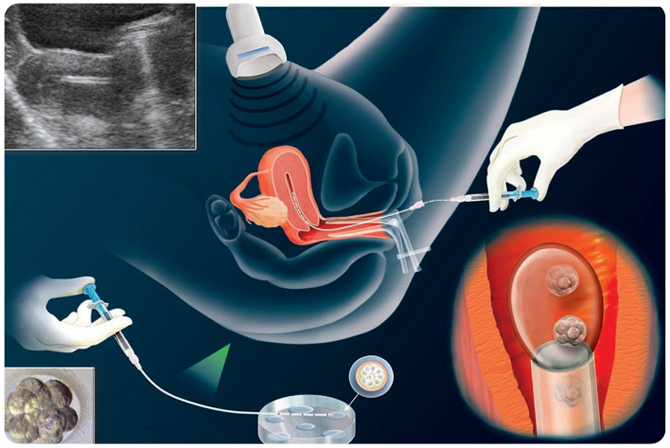
The embryo transfer procedure is the last one of the in vitro fertilization process. It is a critically important procedure. No matter how good the IVF laboratory culture environment is, the physician can ruin everything with a carelessly performed embryo transfer. The entire IVF cycle depends on delicate placement of the embryos at the proper location near the middle of the endometrial cavity. The basic principle of embryo transfer is placement of the embryos to the ideal location in the uterine cavity with as little trauma and manipulation as possible.
The fertilized eggs (now called embryos) are cultured in the laboratory for 1-5 more days and then an appropriate number are selected for transfer to the woman’s uterus. We usually transfer 1 or 2 embryos – see below for more details.
.
Research has been done to determine the optimal location to place the embryos in the uterine cavity. Basically, the middle of the endometrial cavity – half way from the internal os of the cervix to the uterine fundus (top of cavity) – is the best place. Care should be taken to keep the catheter between the top and bottom layers of the endometrium and not to allow it to dissect under the endometrial surface. This is called subendometrial embryo transfer. Pregnancies will occur with subendometrial placement of the embryos, but success rates are lower.
At our IVF clinic, we have the woman lie on her back for 1 hour after embryo transfer before going home. We request that she also limit physical activity for the remainder of that day. This means bedrest after the IVF transfer for the rest of the day and that night. It does not necessarily mean total “bed rest” but can be hanging out on the couch or in the Lazy-boy recliner – watching videos, reading, bossing hubby around, etc. We allow “normal activity” such as working, walking around, etc. beginning the morning after the embryo transfer. Heavy bouncing of the uterus is restricted until after the pregnancy test. Therefore, water skiing, jogging, “uterus bouncing sex”, and other high impact activities are probably not a good idea until after the pregnancy test. Once pregnant, we should be OK do start all that good stuff
For our couples that travel here from out of town for IVF and embryo transfer, we recommend that they do not fly out on the day of the transfer, but wait until the next day. For patients that are driving back home – it is acceptable to drive home (regardless of the length of the drive) after one hour of bedrest in our office following the transfer procedure.
A healthy human embryo will hatch from its shell on day 5-7 after fertilization and implant within hours after hatching out. So actual invasion of the embryo with attachment to the uterine wall occurs about 2-5 days after a day 3 transfer and within 1-3 days after a day 5 transfer.
About 14 days after the transfer, we do a blood test to find out if she is pregnant. If embryo implantation has occurred, HCG hormone will be detectable in the mother’s blood at that time.
How soon can I do a pregnancy test after IVF? We don’t recommend doing a urine pregnancy test (HPT) after IVF. The reason is that there are a lot of falsely negative results. We have seen many beautiful babies born after the wife called us to say that she took a home urine pregnancy test that was negative. A blood test is needed because it is much more sensitive and reliable.
At our IVF clinic, the number of embryos to be transferred is decided by the couple after a discussion with the physician regarding their embryo quality and how it impacts on the risks for multiple pregnancy versus the risk of failing to conceive at all. As female age increases, the implantation rate of the embryos tends to decline. On the baby side of things, a singleton pregnancy is safest. So, in general, we would prefer that only one fetus actually implants and continues development. However, because couples fear failing IVF more than they fear the risks of twins, the large majority at our center decide to replace back 2 embryos when the female partner is under 38, 2 or 3 embryos when she is 38-41, and 3 or 4 (if they have that many) if she is over 41 years old. Transferring this number of embryos seems to result in a “reasonable” balance of high overall pregnancy success rates, and low high-order multiple (triplets or more) rates.