In vitro fertilization (IVF)
Sunflower Hospital is the Best IVF center in India providing the best IVF clinic services and an outstanding Assisted Reproduction India’s best IVF centre located in the Best IVF hospital in India, easily accessible via all forms of transportation.
We understand the life full of challenges that couples face and we try to solve all the challenges that we have learned in all the past years of practice.
IVF is most suitable for couples who desperately want to become parents however none of the conventional ways of managing infertility have worked for them so far. We help fulfill your dream of parenthood by giving the most astounding standard of fertility treatments.
If you are looking for the Best IVF Center India at Sunflower Infertility & IVF Center is the right decision for you. We specialize in all types of fertility treatments for men and women. Our fertility treatments are customized for every patient, utilizing advanced techniques that diminish side effects, stress, and duration of the treatment. Sunflower Hospital is one of the leading infertility hospitals for cost-effective IVF treatment with the best IVF success rates.
sunflower success numbers
1500+
IVF and ICSI procedures a year.
21000+
Live births by IVF and ICSI technology.
Life member
AOGS, AICOG, FOGSI, ISAR, ESHRE, ASRM, IFFS, IMA.
Success rate
70% to 76% in IVF ART.
What Is IVF?
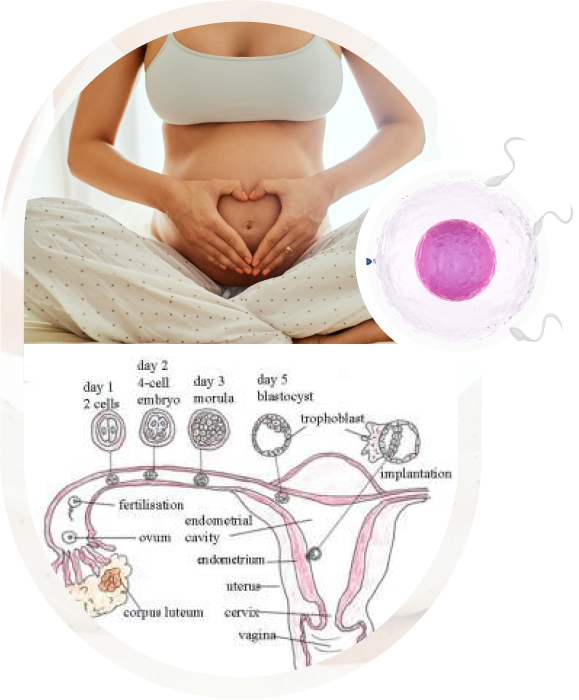
In vitro fertilisation or, what in layman language is better known as test tube baby, involves formation of an embryo in the laboratory by fertilising the female egg and male sperm after retrieving them from the couple. This fertilisation occurs in the tube in the human body in natural conception.
This process involves a series of steps : stimulation of ovaries to produce multiple oocytes -> collection of egg from ovaries -> fertilisation of eggs with partner’s sperm in IVF lab -> embryo culture and grading -> embryo transfer -> pregnancy test 14 days after embryo transfer.
The first “test tube baby”, Louise Brown, was born in 1978 and she herself is a mother of a healthy baby boy now.
Since her birth there are at present nearly 80 lakh children born through IVF.
We are not just a Best IVF clinic in India Sunflower Infertility & IVF Center is a family with specialist doctors, nurses, medical staff, and everyone who works in our hospital to begin someone’s family. Furthermore, we always emotionally support our patients and make them stronger mentally by proper fertility counseling. So that they are ready for treatment without any kind of stress and negative thoughts. This positive way helps us to win half battle.
When Is IVF Indicated
There are a number of reasons for performing IVF

when both tubes are blocked it is not possible for sperm to fertilise egg as the pathway for sperm to reach egg is blocked. Tubal blockage is frequently encountered in patients of genital tuberculosis, pelvic inflammatory disease, moderate or severe endometriosis, previous pelvic surgeries like appendicectomy, ovarian cystectomy, ectopic pregnancy, tubal ligation done for sterilisation.
for natural conception to take place atleast 10 million motile sperm per ejaculate are required. When sperm count & motility is low, sperms are unable to swim upto the egg and hence fertility is impaired.
Rarely the fallopian tubes are found absent since birth. Many causes lead to blockage and damage of tube like severe adhesions, surgical procedures, infections etc.
endometriosis is a disorder which can affect nearly 10% of reproductive age group females. This disorder impacts fertility in a lot of ways like impairment of egg quantity and quality, fertilisation , embryo formation, distortion of pelvic anatomy, uterine receptivity.
once female partner age is more than 38 years all other fertility treatments carry very low success rates, hence IVF being a more successful modality may be considered as first line treatment option in such cases.
in patients with decreased ovarian reserve, ovarian reserve further declines over a period of time. Hence if we wait too long in such patients with the usual fertility treatments such patients may loose out that precious window of time they have to achieve their own genetic child.
when more than 3 IUI cycle have failed in patients with unexplained infertility, IVF becomes a more cost effective and result oriented strategy.
How Is The Procedure Performed?
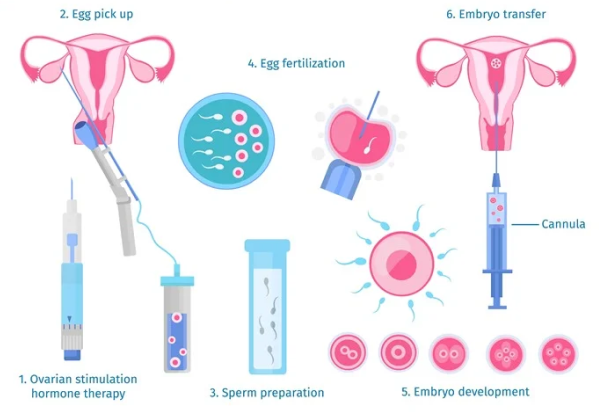
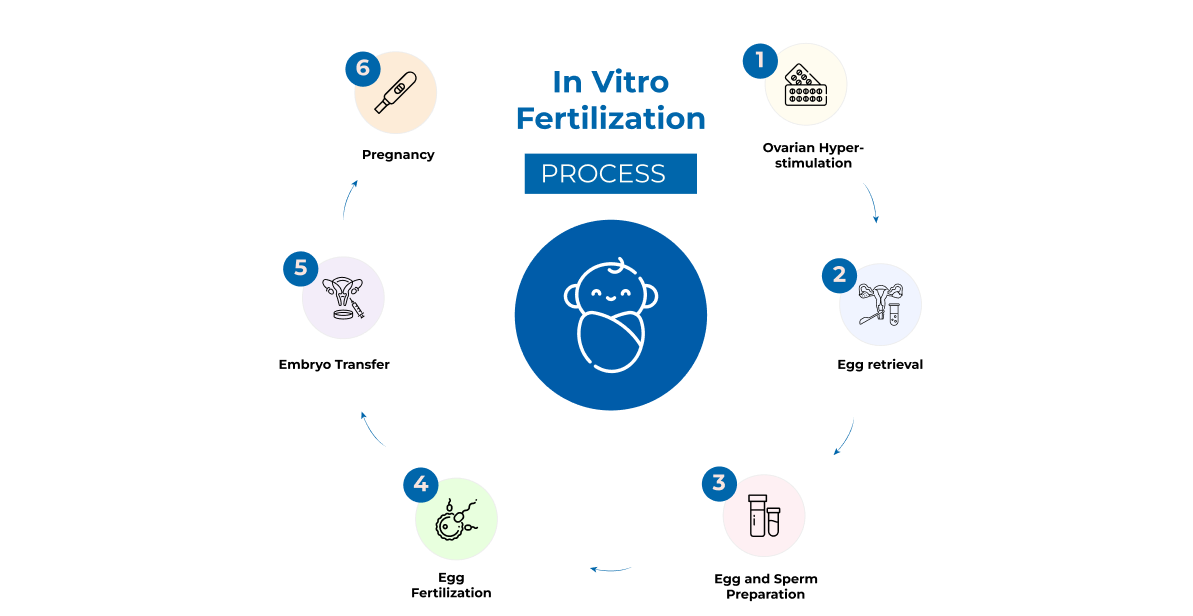
As you can see in the image, IVF is a stepwise process
1) stimulation of ovaries, injections are administered to female partner for 8 -10 days
2) egg retrieval from ovaries, this procedure is performed through transvaginal sonography guided needle aspiration under anaesthesia is a painless procedure with no stich or cut.
3) fertilisation of eggs with partner’s ejaculated ( or surgically retrieved sperm in certain indicated cases) is done in IVF lab through IVF(in vitro fertilisation) or ICSI (intra cytoplasmic sperm injection)
4) embryo maturation, embryos are cultured for 2- 5 days in IVF lab and graded.
5) embryo transfer, 1-2 best grade embryos are transferred back to uterus and rest are frozen.
How to prepare for IVF?
A number of tests are important to plan and prepare for IVF cycle to ensure best results in a single attempt
Ovarian reserve testing

Semen analysis
Mid cycle uterine examination by transvaginal sonography

Infectious disease screening
Certain other tests to fulfil fitness for anaesthesia
Points that will be discussed with you before you undergo IVF
How many embryos should be transferred ?
This is determined based on patient’s age, infertility factor and embryo quality. Older aged women have lower implantation rate, hence older the woman greater number of embryos are transferred, except for women using donor eggs or genetically tested embryos. In a similar way poor quality embryos and certain infertility factors like endometriosis, severe male factor, adenomyosis are associated poorer implantation rate and hence warrant transfer of more embryos. However risk of multiple pregnancies should be weighed.
What will you do with any extra embryos?
Excess good grade embryos are cryopreserved for patient’s further use if necessary for second pregnancy or next embryo transfer in case first one fails. Not all embryos will survive the thawing process, although 99% will.
Cryopreservation can make future cycles of IVF less expensive and less invasive. Certain patients who deliver healthy twins or those who donot want further pregnancy choose to discard unused embryos.
How will you handle a multiple pregnancy?
Transfer of 2 or more embryos poses you at a risk of multiple pregnancies, nearly 30 -50% concieve a twin pregnancy via IVF.
IVF Process
- 1. Ovulation induction
- 2. Egg retrieval
- 3. Sperm retrieval
- 4. Fertilisation
- 5. Embryo transfer
- 6. Pregnancy testing
In IVF hormones are injected to stimulate your ovaries to produce multiple eggs — rather than the single egg that normally develops each month. Multiple eggs are needed because few eggs might not fertilise, few embryos may arrest or may be of poor grade.
Medications given are :
- for ovarian stimulation.To stimulate your ovaries, we administer injectable hormones like FSH ( follicle stimulating hormone ) and LH ( leutinising hormone).
- for oocyte maturation.Once follicles are mature, trigger injection is adminsitered like human chorionic gonadotropin (HCG) or GnRH agonist to help achieve final oocyte maturation.
- to prevent premature ovulation.GnRH antagonists like cetrorelix / ganirelix or GnRH agonists like lupride or gonapeptyl are administered to prevent premature ovulation or premature progesterone rise.
- Ovarian stimulation usually lasts for about 8-14 days.
- To determine when the eggs are ready for collection, we perform:
- Vaginal ultrasound,an imaging exam of your ovaries to monitor the development of follicles — fluid-filled sacs where eggs mature
- Blood tests,to measure your response to ovarian stimulation medications — estrogen levels typically increase as follicles develop, and progesterone levels remain low until ovulation
IVF Cycle Cancellation
IVF Cycle may be cancelled it ovaries are not responding too well.
- Inadequate number of follicles developing
- Premature ovulation
- No eggs retrieved during egg retrieval
- Failure of fertilisation
- No embryos formed
- Other medical issues
- Egg retrieval is done 34 to 36 hours after the final injection and before ovulation.
- For egg retrieval you shall be admitted at about 8-9 am on an empty stomach.
- Egg retrieval is performed under general anaesthesia.
- Transvaginal ultrasound aspiration is the usual retrieval method. An ultrasound probe is inserted into your vagina to identify follicles. Then a thin needle is inserted into an ultrasound guide to go through the vagina and into the follicles to retrieve the eggs.
- The follicular fluid is aspirated through a needle connected to a suction device. Multiple eggs can be removed in about 20 minutes.
- After egg retrieval, patient may experience mild lower abdominal pain or minor vaginal bleeding.
- Follicular fluid is then screened for cumulus oocyte complexes(COCs). For IVF eggs that appear healthy and mature will be mixed with sperm to attempt to create embryos. However, not all eggs may be successfully fertilized. ) For ICSI, COCs are incubated for 2 hours, following which they are stripped, metaphase 2 oocytes are then injected with sperms.
After the procedure
After the egg retrieval , you can resume normal daily activities. However, your ovaries may still be enlarged. Consider avoiding vigorous activity, which could cause discomfort.
It is observed that post OPU there is minor discomfort like cramping :
- Mild vaginal spotting
- Breast tenderness
- Mild bloating
- Mild lower abdominal pain
- Constipation
- If you develop moderate or severe pain or heavy bleeding after egg retrieval , contact us. You will be evaluated for complications such as infection, twisting of an ovary (ovarian torsion) and severe ovarian hyperstimulation syndrome.
Your partner will be asked to produce a semen sample through masturbation. Sperm will be seperated from seminal plasma. In certain cases like when partner diagnosed with azoospermia ( zero sperm count ), sperms can be retrieved by needle aspiration from epididymis or testis.
Fertilization
Fertilization can be attempted using two common methods:
Conventional insemination:
During conventional insemination, healthy sperm and mature eggs are mixed and incubated overnight.
Intracytoplasmic sperm injection (ICSI):
In ICSI, a single healthy sperm is injected directly into each mature egg. ICSI is often used when semen quality or number is a problem or if fertilization attempts during prior IVF cycles failed.
- Embryo transfer is performed 2 to 5 days after ovum pickup.
- The procedure is usually painless and doesn’t require anaesthesia in most cases.
Embryos are inserted via a long, thin, flexible tube called a catheter into your vagina, through your cervix and into your uterus. - A syringe containing one or more embryos suspended in a small amount of fluid is attached to the end of the catheter.
- Under trans abdominal sonography guidance once catheter is placed at proper position, embryos are injected.
- If successful, an embryo will implant in the uterus about 2 -5 days after embryo transfer.
About 14 days of embryo transfer ,we will test a sample of your blood to detect whether you’re pregnant.
If you’re pregnant,we will ask you to continue the medications and schedule you for an ultrasound after 4 weeks of embryo transfer.
If you’re not pregnant,you’ll stop taking progesterone and likely get your period within a week. If you so it seems like you have frozen embryo remaining with us , we will guide you through the next cycle. We will perform a few tests to determine cause of failure and apply a few more modifications to improve your chances of getting a pregnancy.
What is “Freeze-All Cycle” and OHSS-Free Clinic?
Freez all embryos and OHSS free clinic.
Ovarian hyperstimulation syndrome is a major iatrogenic complication of ovarian stimulation, performed for assisted reproductive technology. Ovarian hyperstimulation syndrome (OHSS) is a potentially life-threatening condition with massive ovarian enlargement, ascites, hydrothorax, liver dysfunction, and renal failure. OHSS can lead in 2% to hospitalization.
We have to change totally the concept of IVF to obtain an OHSS Free Clinic which is segmentation of IVF treatment in following steps:
- ovarian stimulation with agonist triggering avoiding OHSS
- vitrification of all oocytes and/or embryos
- single or double embryo transfer after thawing in a receptive endometrium in next cycle.

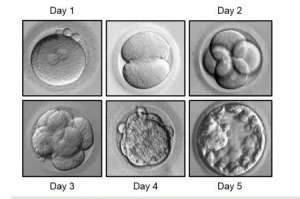
Extended embryo culture in IVF lab
Embryo cannot survive beyond 5-6 days of culture in the IVF lab, and hence are frozen at that stage and later warmed before transfer when conditions are optimised.
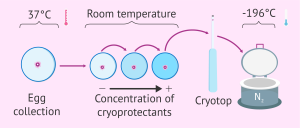
Vitrification (freezing) technique
Embryos are frozen with vitrification technique, that is a technique which involves replacing all the water from the cells with cryoprotectant and then subjecting it to a temperature as low as -196 degree celsius which leads to glass like freezing.
Post warming survival rate
This technique has very good post warming survival rate of embryos as high as 99-100% as no ice crystals are formed, like in slow freezing technology which was use a couple of years back.

Success rate of freeze all cycles
Since 2017 we have adopted the all freeze cycle approach, this has helped us achieve consistently higher pregnancy rates ( >10-15%) than fresh embryo transfer cycles except for a few select cases where we perfrom fresh embryo transfer.
Safety of embryo freezing
This process is absolutely safe procedure for both patient and her child. Children born thus are not known to have any high risk of abnormality.
Advantages
- It nullifies risk of ovarian hyperstimulation syndrome
- Embryo transfer can be planned as per patient’s convenience.

What Is The Success Rate?
With multiple IVF centers and clinics mushrooming across the country, it can become quite confusing to select the right IVF centre to undergo the IVF cycle as a patient.
One of the cornerstone in guiding the couple’s decision to chose the right IVF clinic is the clinic’s success rates Here we present to you our IVF success rates per embryo transfer and cycle numbers over the last 10 years.
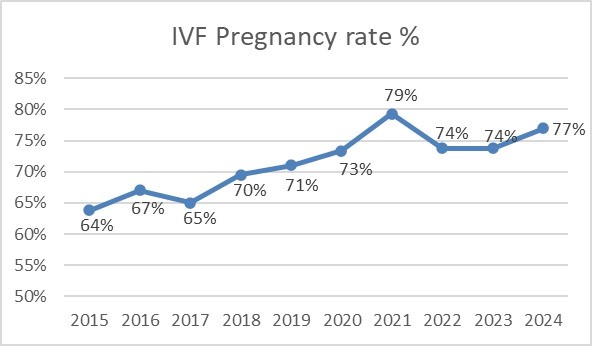
What Is The Cost Involved?
- The IVF Cost involved for IVF has remained nearly the same for the last 10 years.
- The cost is dependant on the type of injection used for IVF stimulation, the kind of IVF lab set up, and consumables.
- Compromising on quality does bring down the cost but at the sacrifice of success rates.
- However, an IVF cycle in India cost is nearly 1/10 of that USA, UK, Australia, etc.
- The success rate of India’s best IVF centre in our clinic is similar.
- Hence India is becoming a medical tourism hub for IVF treatment

